Joint Pain in the Elderly: Causes, Risks, Prevention, and Treatment

Joint Pain in the Elderly: Causes, Risks, Prevention, and Treatment Facebook Twitter Youtube Instagram As we age, joint pain becomes our regular companion, and not to forget that once it sets in, the damage can’t be undone, but can only be managed. Pain showing up as we age is common, but it can be delayed if we are vigilant and alert during our mid-years by choosing a healthy lifestyle and diet. According to the University of Michigan National Poll on Healthy Aging, 70% of adults over 50 experience joint pain at least occasionally, and 60% have been diagnosed with some form of arthritis. Nearly half of those with arthritis report daily pain (45%), and about 49% say joint pain limits their usual activities to some extent. Over a third (36%) find that it interferes with their daily life. Let’s uncover more about joint pain causes and how joint pain treatment works. You may not feel it until you fracture it: How to work around joint pain? Bone loss happens as we age, and certain conditions trigger it. For instance, in women, it speeds up after menopause. The tricky part is you don’t feel it happening; you are going about your day, and a sudden twitch, a snap, that’s it. Your bones are your supportive bestie, always holding you up, but sometimes your bestie can’t offer you all. That’s where the unchecked bone loss kicks in with signs. What is Arthritis and How is it Different from Osteoarthritis? While the terms ‘osteoarthritis’ (OA) and ‘arthritis’ are sometimes used interchangeably, they aren’t synonymous. Arthritis encompasses over 100 joint conditions characterized by inflammation, affecting both the joints and surrounding connective tissues. Osteoarthritis is a specific type of arthritis, often referred to as degenerative or wear-and-tear arthritis, because it results from long-term joint usage as people age. Osteoarthritis results from cartilage breakdown at the ends of bones where joints form, leading to pain and stiffness. It’s the most common form of arthritis, affecting 32.5 million adults in the United States, and is followed by rheumatoid arthritis (RA) an inflammatory type that can damage joints and organs. Globally, osteoarthritis is a leading cause of disability. Common Symptoms of Osteoarthritis Pain in affected joints, worse after activity or long days Stiffness, especially after rest or inactivity, improves with movement Tenderness and general discomfort Reduced range of motion and loss of flexibility Crepitus – grating, clicking, or popping sounds during joint movement Bone spurs – extra bone at joints, may form visible lumps Swelling in the tissues surrounding the joints as OA progresses Frequently Affected Joints Knees: Pain, difficulty walking, climbing stairs, getting in/out of bed Hips: Pain in the hip, groin, inner thigh, buttocks, or knees; reduced mobility Other areas: Shoulders, hands, fingers, feet Spine: Neck and lower back pain/stiffness Pressure on spinal nerves causing: Weakness Numbness Tingling in arms/legs Severe cases: bowel/bladder dysfunction Types of Joint Pain Wrist Joint Pain Wrist pain commonly arises from repetitive strain, sprains, or underlying conditions like carpal tunnel syndrome. It may gradually impact movement and fine motor control. Knee Joint Pain Often linked to overuse, injury, or degenerative issues like osteoarthritis, knee joint pain can affect mobility and stability in everyday activities. Finger Joint Pain Pain in the finger joints may be due to inflammatory diseases such as rheumatoid arthritis or gout. It causes stiffness, swelling, and difficulty with precise tasks. Hip Joint Pain Hip joint pain may result from age-related cartilage wear, bursitis, or muscle strain. It often limits motion and may spread to nearby areas like the thigh or groin. Hand Joint Pain Hand joint discomfort often stems from arthritis or repetitive use injuries. It can make gripping or performing routine tasks painful and difficult. Leg Joint Pain Leg joint pain may originate from issues in the hip, knee, or ankle, or be related to nerves. It can vary in intensity and often worsens with prolonged activity. What are the Notable Joint Pain Causes? Injury Joint damage can result from falls, sprains, overuse, or strain on tendons and ligaments. Common injury sites include the shoulder, knee, hip, wrist, and ankle. Osteoarthritis (OA) Caused by the gradual breakdown of cartilage due to aging or joint stress. More common in older adults, especially those with excess weight, prior joint injuries, or a genetic predisposition. Autoimmune Diseases Includes conditions like rheumatoid arthritis, psoriatic arthritis, and lupus, where the immune system mistakenly attacks joint tissues. Often begins in younger adults and disproportionately affects women. Gout (Crystalline Arthritis) Triggered by high uric acid levels, leading to sharp crystals forming in joints—most frequently the big toe. Often linked to dietary habits and genetic susceptibility. Pinched or Inflamed Nerve Occurs when nerves supplying the joint are compressed or irritated. Examples include carpal tunnel syndrome (wrist pain) and spinal nerve compression (hip pain). Joint Infection Though rare, infections spreading through the bloodstream can invade joints, causing sudden pain, swelling, redness, and systemic symptoms like fever or chills. Joint Pain Treatment A combination of lifestyle modifications and targeted therapies is apt for osteoarthritis. Guidelines for joint pain treatment highlight the importance of weight loss, regular exercise, and participation in self-management programs led by arthritis educators. Complementary approaches such as tai chi, yoga, cognitive behavioral therapy, acupuncture or acupressure, and the use of braces, splints, Kinesio taping, and topical treatments like heat, cold, or pain relievers are also encouraged. Despite these recommendations, while 64% of individuals with joint pain report engaging in exercise and 24% have undergone physical therapy, fewer utilize non-drug strategies such as braces. In terms of medication, the focus remains on short-term use of over-the-counter pain relievers at the lowest effective dose, alongside steroid joint injections for selected cases. As regards workout inclusion, it is advisable to add bone-strengthening exercises to your routine, like walking, resistance band workouts, or light weight training. A simple and consistent workout routine will do wonders. You might feel fine today, but that doesn’t always mean your joints are thriving. Osteoarthritis often whispers before it shouts. So, listen
Everything You Need to Know About ACL Injuries

Everything You Need to Know About ACL Injuries Facebook Twitter Youtube Instagram Not just athletes, but anyone can suffer from Anterior Cruciate Ligament (ACL) injuries. So, what exactly happens when this ligament gets injured? How does it tear, and how can you tell if that’s what you’re dealing with? We’ll break down how ACL injuries happen, what symptoms to watch for, and answer some of the most common questions we hear. What is an ACL injury? An ACL injury results from an ACL tear in your knee. It is one of your knee ligaments and connects your thigh bone (femur) to your shin bone (tibia). An ACL forms an “X” shape inside your knee with your posterior cruciate ligament (PCL). While an ACL is closer to the front of the knee, a PCL is closer to the back of it. Imagine ACL is like a strap that connects your bones and prevents your knee from bending or rotating too much. An ACL injury happens because of sudden high intensity force to the knee that bends or twists it farther than its natural limit. Types of ACL Knee Injuries Grade 1: The injury stretched your ACL enough to damage it, but it’s still in one piece and holding your knee bones together. Grade 2: The injury stretched your ACL so much that it was partially torn and loosened. Grade 3: A complete tear of your ACL is in two pieces. What are ACL Injury Symptoms? Common signs of an ACL injury include: A popping sound or sensation in the knee Swelling shortly after the injury Pain, especially when putting weight on the knee Feeling of instability or the knee “giving out” Reduced range of motion in the knee What Causes ACL Tears? ACL tears occur when excessive force or unnatural movement strains the knee beyond its limits. This often happens when the knee twists or shifts too suddenly. Typical causes of ACL Injury include: Sports injuries Car accidents Slips and falls Who is at Risk for ACL tears? ACL injuries can affect anyone, but they’re most common among athletes, especially those in sports with quick stops, twists, and direction changes, such as: Soccer Football Basketball Gymnastics Lacrosse What to Expect During Your Doctor’s Visit for an ACL Injury Your first appointment typically starts with a detailed conversation. Your doctor will ask about your symptoms, how the injury happened, and your medical history to get the full picture. Then comes a hands-on exam, where your doctor will carefully check your injured knee, comparing it to the other side. Most ligament injuries, including ACL tears, can be identified just through this thorough physical examination. Imaging That Might Be Used To confirm what’s going on or rule out other issues, your doctor might suggest: X-rays – While they can’t show ligament damage, X-rays help spot any related bone injuries. MRI scans – These give a clearer look at soft tissues, including your ACL, meniscus, and cartilage. MRIs aren’t always necessary to diagnose a tear, but they can be useful to see if anything else in the knee is affected. What are the Treatment Options for an ACL tear? Treatment depends on your lifestyle, activity level, and overall health. Active individuals and athletes, especially those in agility-based sports, often need surgical reconstruction to restore stability and safely return to competition. Less active or older adults may recover with non-surgical treatment, such as physical therapy and lifestyle adjustments, especially if their daily activities don’t require intense knee movement. There are two main approaches to ACL Injury Treatment: repair and reconstruction. ACL Repair This is a less common option and only suitable for very specific cases, typically when the ligament has cleanly torn off from the bone. It’s mostly used in acute injuries and select patients. ACL Reconstruction This is the gold standard for most people. It involves replacing the torn ligament with a graft, which could be: Autograft – using your own tendon (usually patellar, hamstring, or quadriceps tendon) Allograft – using donor tissue (more common in older or less active patients) Who Should Think About ACL Reconstruction Surgery? If you’re an active adult, playing sports that involve quick moves, twists, or heavy lifting at work, ACL surgery might be a smart option. Even older adults can benefit from surgery if they stay physically active. For kids and teens, surgery needs extra care. Their bones are still growing, so doctors weigh the risk of growth problems. But research shows that delaying treatment can lead to more damage inside the knee, like tears in the meniscus or cartilage. If your knee feels unstable and keeps giving way, you may be at risk of injuring other parts of your knee, making surgery a stronger recommendation. Sometimes, ACL injuries happen alongside other knee damage, like: Meniscus tears Cartilage damage Ligament sprains (like MCL) This combo, especially common in sports like football and skiing, is called the “unhappy triad.” In these cases, surgery often helps everything heal better, especially if meniscus repair is done at the same time. Rehabilitation After ACL Surgery Physical therapy plays a critical role in recovering from ACL surgery, often starting right after the procedure. The key to a strong recovery lies in your commitment to rehab. Thanks to modern surgical methods and secure graft fixation, recovery is now faster and more focused than it used to be. The First Few Days Post-Surgery During the first 7 to 10 days, your priority is to: Keep the surgical site clean and dry Begin gentle exercises to straighten the knee and activate the quadriceps Icing your knee regularly helps ease pain and swelling. Your surgeon might recommend a brace or a passive motion machine to help you bend and extend your knee, though studies show the machine isn’t essential for a good outcome. Whether you use crutches and how much weight you put on your leg will depend on your surgeon’s advice and whether other injuries were treated during surgery. What Rehab For ACL Injury Aims to
What Is a Hairline Fracture? Causes, Symptoms, and Treatment Options
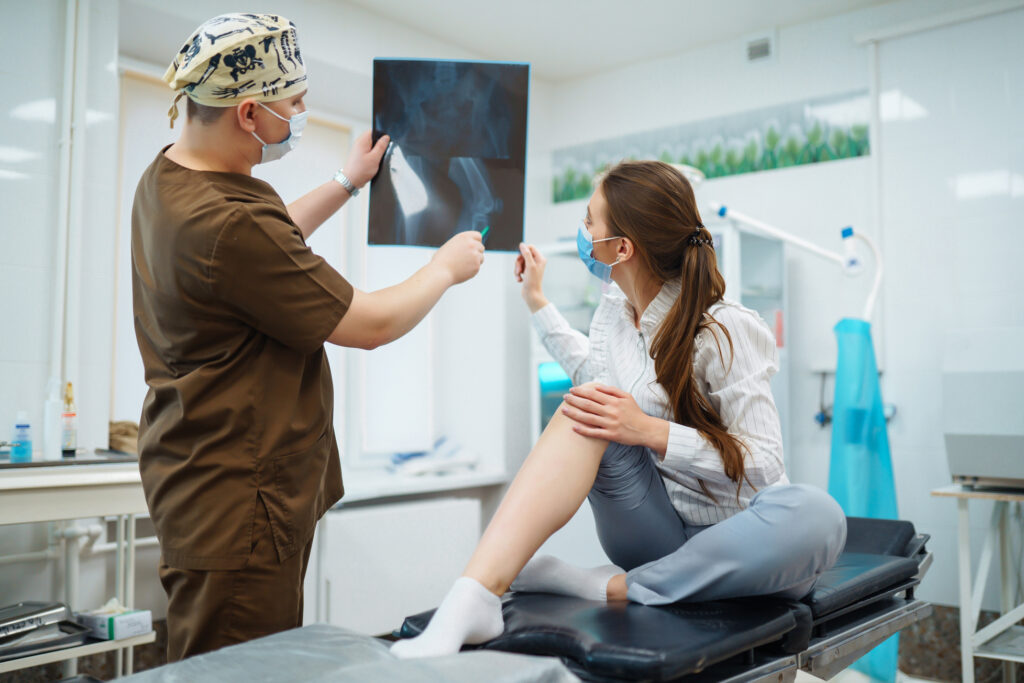
What Is a Hairline Fracture? Causes, Symptoms, and Treatment Options Facebook Twitter Youtube Instagram Not all injuries show themselves right away. Sometimes, even without swelling or bruising, a nagging pain lingers, especially after repetitive movements or a recent increase in physical activity. You might brush it off as a minor sprain or overuse. But when the pain doesn’t go away, it’s worth considering a deeper cause. In many cases, this kind of ongoing discomfort turns out to be something like a hairline fracture. In this blog, we will explain what hairline fractures are, what causes them, how to recognize the symptoms of a hairline fracture, and what treatments are available for a smooth recovery. What is a Hairline Fracture? Hairline fractures are usually caused due to repetitive trauma or overuse. A hairline fracture is an extremely small fracture that, at first, might not be seen on an X-ray, including in early stages. Hairline fractures are most typically seen in sports where there are multiple repetitions or impacts on particular areas of the body, such as basketball, running, gymnastics and dance. Risk Factors for Hairline Fractures Certain risk factors increase your risk of developing hairline fractures: Gender: Women are at an increased risk for hairline fractures, especially if they have irregular menstrual cycles. Anatomical Concerns: Flat feet, high arches, or poor-quality shoes may potentially add extra stress to bones. Bone Health: Certain disease states, like osteoporosis, ultimately lead to weakened bones and an increased risk of fractures. History of Fractures: If someone had one hairline fracture in the past, it raises their risk of having additional hairline fractures in the future. Nutrition: A lack of calcium or vitamin D compromises bone strength, raising fracture risk. What are the Causes of Hairline fractures? Multiple things can lead to hairline fractures, which are as follows: 1. Repetitive Activity Participating in a high-impact sport or repeatedly running can place excessive stress on the same bones over and over, and lead to microfracture injury. 2. Sudden Increase in Activity Regularly living your normal lifestyle and suddenly beginning an aggressive exercise plan raises the chances of a fracture. 3. Improper Footwear Using old or improper shoes (especially with high-impact exercise) can put too much stress on your foot and ankle bones. 4. Poor Nutrition Not receiving enough calcium, vitamin D or calories makes them more prone to fractures. 5. Underlying Conditions Osteoporosis or other conditions that deteriorate bone health can make bones more brittle, causing them to break with even the smallest amount of stress. What are Hairline Fracture Symptoms? Hairline fracture symptoms can be subtle at first and progress over time. They can often look like other soft tissue injuries that will require a diagnosis. Watch for: Localized pain that intensifies through activity and diminishes with rest. Swelling or tenderness in the area of the injury. Some bruising. Difficulty bearing weight or completing certain movements. In the ankle or foot, observe a limp or an inability to walk comfortably. In the wrist or hand, notice weakness while gripping or lifting an object. Common Hairline Fracture Areas and How to Identify Them 1. Hairline Fracture in Foot Often called the metatarsal bones (top of the foot). Seen frequently with runners and athletes. Symptoms: Pain on the top or side of the foot, especially while walking Treatment: Rest, supportive shoes, or a walking boot 2. Hairline Fracture Ankle The level of injury often depends on a sudden twist or repeated use. High-risk groups are runners and basketball players. Symptoms: Sharp pain around the ankle joint, swelling Treatment: elevate, ice, and partially immobilize with a boot or splint 3. Hairline Fracture Leg It will often involve the tibia (shin bone), especially for long-distance runners or repeated jumpers. Symptoms: dull pain, especially with pressure Treatment: strict rest, anti-inflammatory medication, sometimes cast. 4. Hairline Fracture Knee Usually rare, it occurs in the patella (kneecap) or femur (thigh bone). Symptoms: restrictions in bending the knee, stiffness, pain with bending and walking Treatment: consequential support and physical therapy post-rest period. 5. Hairline Fracture Wrist Caused by an acute fall or constant use (e.g. weightlifting or typing). Symptoms: Pain when using the wrist or applying pressure Treatment: Displaced or non-displaced wrist splint or cast, and activity modification. 6. Hairline Fracture Hand Most commonly seen in athletes or fall hacks, it will usually involve the metacarpal bones. Symptoms: Pain when gripping or making a fist Treatment: Immobilization using a splint or short cast Diagnosis: Do You Need an X-ray? Hairline fractures may be hard to detect on initial X-rays, especially in the first week after the injury. If a fracture is suspected but unconfirmed, physicians might recommend the following imaging with the understanding that for most bone injuries it will likely take time for swelling or changes that may suggest healing or otherwise to be indicated: MRI scan: best for soft tissues and identifying fractures early Bone scan: will show changes in bone metabolism CT scan: for complicated or deep fractures So, if you have continued pain and are wondering if it’s a sprain, don’t disregard it. Hairline Fracture Treatment Options Are you anxious that your bothersome discomfort could be more than a sprain? If you have been told that you have a hairline fracture, you may be wondering, “Do I need a cast? Will this heal by itself? When will I feel back to normal?” Fortunately, most hairline fractures resolve quickly and with appropriate care. However, understanding what to do and not to do while you are recovering can be key. Below are safe and effective ways to treat a hairline fracture. The treatment of a hairline fracture starts with R.I.C.E., which means Rest, Ice, Compression, and Elevation to help minimize swelling and prevent further damage. Depending upon the location of the fracture, our specialists/ doctors may use splints, walking boots, and braces to immobilize the area. If the fracture is in the foot, ankle, or leg, crutches may be necessary to help keep all weight off the bone. Pain management is
Why Choose MJ Naidu Hospital for Your Knee Replacement? Introducing the Pixee Medical Knee+ System
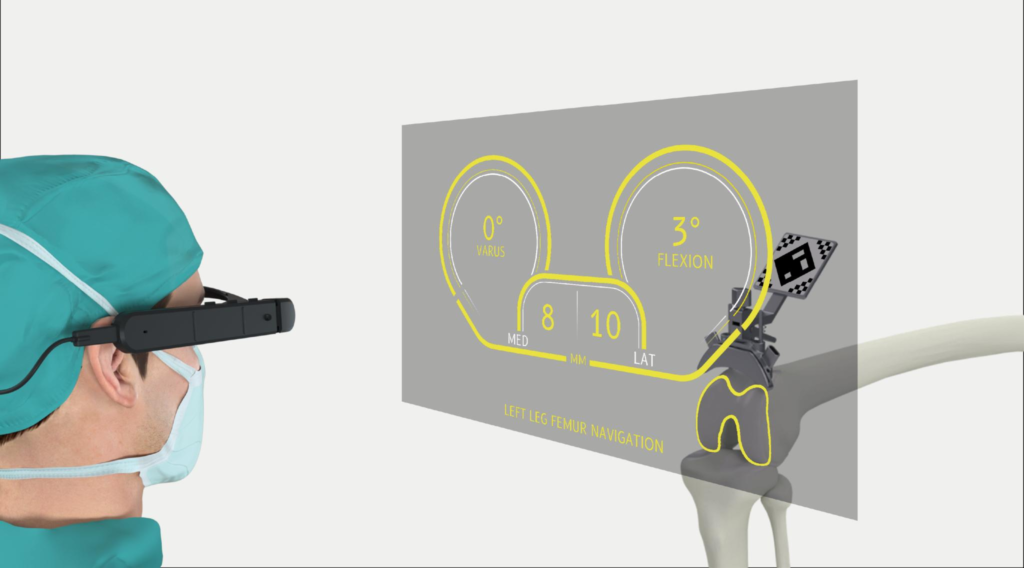
Why Choose MJ Naidu Hospital for Your Knee Replacement? Introducing the Pixee Medical Knee+ System Facebook Twitter Youtube Instagram With the recent developments in MedTech, knee replacement surgeries have undergone a shift from the early traditional approach. AR technology has been the trailblazer, providing more anatomic information for each patient, allowing surgeons to be precise and perform cuts to the specific anatomy. This will translate to better outcomes for the patients as opposed to the past methods of a one-size-fits-all solution. MJ Naidu Hospital is proud to introduce the revolutionary Pixee Medical Knee+ system, marking a significant advancement in our commitment to precision-driven surgical care. Let’s dive more deeply into how this cutting-edge AR technology is shaping the future of knee replacement surgery. What Is the Pixee Medical Knee+ System? The Knee+ is an innovative augmented reality solution specifically designed for total knee arthroplasty procedures. This system provides real-time navigation of angular values and resection levels, helping surgeons achieve implant positioning accuracy with robotic-like precision. The system features a redesigned interface combined with high-precision surgical tools to provide seamless, personalized guidance throughout the procedure. What sets the Knee+ apart is its intuitive design that allows surgeons to maintain complete control while benefiting from advanced AR visualization. Key Advantages of the Knee+ System: Surgeon-Controlled Precision: The system allows surgeons to accurately align the position of total knee components through a completely surgeon-controlled headset, miniaturizing and streamlining total knee surgery with a very small back table footprint. No Pre-Operative Scans Required: The augmented reality system integrates into existing workflows and requires no pre-op scans while achieving implant positioning with robotic-like precision. Proven Track Record: The system has already been used in over 10,000 procedures in more than 20 countries, demonstrating its reliability and effectiveness. FDA-Cleared Technology: The Knee+ has received FDA 510(k) clearance, ensuring it meets the highest safety and efficacy standards for surgical navigation systems. What Is Augmented Reality in Knee Surgery? Augmented Reality (AR) in knee surgery brings digital technology right into the operating room, giving surgeons a real-time, view of your knee as they work. With the Knee+ system, you can think of it as a high-tech overlay that guides each step, helping ensure your knee implant is placed with incredible accuracy, tailored to your unique anatomy. Why It Matters for You: Smaller incisions for less surgical trauma and faster healing Pinpoint precision helps ensure a better fit and more natural movement Shorter recovery times to help you get back on your feet sooner Enhanced surgical accuracy without the need for additional pre-operative imaging AR vs. Robotic-Assisted Knee Surgery: Understanding the Difference While both technologies aim to improve surgical outcomes, there are fundamental differences between augmented reality systems like the Pixee Medical Knee+ and traditional robotic-assisted surgery systems currently available in the market. Current Robotic Systems in the Market: MAKO SmartRobotics (Stryker): A semi-active robotic arm-assisted system that relies heavily on preoperative CT imaging for surgical planning. The MAKO system only captures virtual gap data in full extension and 90° of flexion. ROSA Knee System (Zimmer-Biomet): A semi-active robotic arm-assisted system that offers touchscreen interface and continuous visual feedback. However, recent studies have shown unsatisfactory accuracy in calculating certain critical angles. VELYS Robotic-Assisted Solution (Johnson & Johnson): Designed to work in conjunction with ATTUNE Knee System implants, focusing on increased accuracy and precision. CORI Surgical System (Smith & Nephew): Another semi-active robotic arm system with touchscreen capabilities. Comparative Advantages of AR Systems vs. Robotic Systems: Feature Pixee Medical Knee+ (AR) Traditional Robotic Systems Pre-operative Requirements No CT scans required Require preoperative CT imaging Setup Complexity Minimal setup, small footprint Large robotic arms, extensive setup Surgeon Control Complete surgeon control Semi-active assistance with some limitations Workflow Integration Seamless integration May require workflow modifications Clinical Outcomes Comparison: AR System Advantages: The Pixee Medical Knee+ system achieves similar precision outcomes without the complexity, cost, and pre-operative imaging requirements of robotic systems. Some studies suggest cost savings in episode-of-care costs with advanced surgical systems. Why Choose AR Over Robotic Systems? Accessibility: No need for expensive pre-operative CT scans makes the procedure more accessible to patients. Efficiency: Streamlined workflow without the setup time required for robotic arms and extensive calibration. Surgeon Autonomy: Maintains complete surgeon control while providing precision guidance. Adaptability: Can be integrated into existing surgical workflows without major infrastructure changes. What are the steps involved in using the Knee+ AR Technology? Unlike traditional approaches or even standard robotic systems, the Knee+ system enhances the surgeon’s capabilities with real-time, data-rich visualization and decision-making tools while maintaining complete surgeon control. Here’s how this advanced system works from start to finish: Step 1: Streamlined Setup The Knee+ system requires minimal setup with its compact design and small back table footprint. Unlike traditional systems, no pre-operative CT scans or extensive planning sessions are required, making the process more efficient for both patients and surgical teams. Step 2: Real-Time Calibration During surgery, the system performs real-time calibration using the patient’s anatomical landmarks. The cutting planes are oriented with respect to the mechanical axes of the patient and are calculated specifically for each individual case. Step 3: Sensor-Driven Navigation Small sensors provide dynamic feedback while allowing the surgical team to move freely. The system offers precise navigation of angular values and resection levels throughout the procedure, ensuring optimal implant positioning. Step 4: Enhanced AR Visualization Wearing the AR headset, the surgeon sees an overlay of the patient’s anatomy and surgical data directly in their field of view. This setup eliminates the need to glance away at external monitors, creating a more intuitive and immersive operating environment. Measurements, alignment guides, and positioning data appear layered over the actual knee, improving both confidence and accuracy. Step 5: Precision-Guided Bone Cuts The AR system guides precise bone cuts that are tailored to the patient’s unique anatomy. The surgeon maintains complete control while benefiting from real-time feedback and guidance, ensuring optimal implant fit and alignment. Step 6: Functional Optimization The system integrates functional measurements and ensures proper ligament tension and soft
Elderly Fall Prevention: Common Causes and Tips to Reduce Fall Risk at Home

Elderly Fall Prevention: Common Causes and Tips to Reduce Fall Risk at Home Facebook Twitter Youtube Instagram Did you know that one in four adults aged 65 and older experiences a fall every year? One trip over the carpet or the slippery bathroom can put a hold on your active life. Moreover, a fall not only results in discomfort but also it can also trigger serious health problems, leading to long-term disability. The risk of falling and fall-related problems rises with age, making fall prevention your top priority. Exercising, managing medications, regular check-ups, and incorporating other elderly fall prevention tips can reduce fall risks. Due to fear of falling, many older adults avoid activities such as walking or taking part in social activities. On the other hand, staying active is important to keep your body healthy and physically active. Keep the fear of falling at bay by learning the causes of falls in the elderly, addressing the potential fall risks, and making your home spaces better planned for ease of movement. Causes of Falls in the Elderly Falls in older adults can result from a complex interplay of physical, medical, and environmental factors. Understanding these contributors is essential for effective elderly fall prevention. As we grow older, natural changes such as decreased vision, diminished hearing, and slower reflexes make it harder to notice and respond to hazards in time. These sensory and cognitive shifts significantly elevate fall risk, even during routine daily activities. Chronic health conditions, including diabetes, heart disease, thyroid problems, and disorders of the nervous system, blood vessels, or feet, can subtly interfere with balance and coordination. When multiple conditions like this are present, they may compound and further increase an older adult’s likelihood of falling. The urgency caused by incontinence or other bladder and bowel issues can lead to rushed movements, especially at night. This haste, combined with fatigue, darkness, or cluttered pathways, contributes to unsafe situations and adds another layer of concern for elderly fall prevention. Cognitive changes, such as mild cognitive impairment or certain types of dementia, may lead to forgetfulness, poor judgment, and disorientation. These challenges can interfere with decision-making and spatial awareness, putting older adults at a higher fall risk even in familiar environments. By addressing these issues proactively, elderly fall prevention efforts can significantly improve safety, independence, and quality of life for older adults. A well-rounded approach to elderly fall prevention involves assessing health, reviewing medications, modifying living spaces, and promoting strength and balance exercises. You may be interested to know – Hairline Fracture https://youtube.com/shorts/zWQzyRcMkF0?feature=shared Six Tips for Fall Prevention It is important to take care of your health overall to lower the chance of a fall. Mostly, falls and accidents don’t happen without reason; if taken care they can be prevented. Src:NIH Stay physically active: One must plan an exercise program and be consistent. Exercises help keep joints, tendons, and ligaments flexible and strong. Lightweight bearing exercises paired with regular walking are a good start. The aim is to strengthen the bones and muscles to avoid injuries and other conditions. Strengthening and balancing exercises improve the overall coordination and muscle strength. Yoga is a good start, paired with tai chi. Incorporating resistance bands is also an added advantage. For older adults, activities such as squatting, standing up from a chair and walking may be difficult or cause them to feel unsteady, which increases their fall risk. Exercises such as sit-to-stand exercise, balancing exercises increase their mobility reflex and reduce the fall risk. One must also consider fall-proofing the home to ensure safety. Fall prevention tips such as keeping corners and spaces free of clutter, non-slippery tiles, lighting up the spaces well, making clear paths to switches, removing unnecessary things from the walkways, etc, can help in fall prevention. It is equally important to have regular checkups like hearing and sight, as the slightest changes, if left unnoticed, can cause trouble. If you are opting for new glasses, take time to adjust to them and make sure it doesn’t cause you any discomfort. Overall, medical checkups should also be in your fall prevention strategy, as it is important to monitor whether any ongoing medication needs to be changed or modified. One of the most common reported causes is the sudden getting up from the bed after sleeping. This must be avoided at any cost, as sometimes when you get your reflexes are still not fully active. Take time and don’t ignore the signs your body is giving. Assistive devices are a good add-on. Your doctor might recommend using a cane or a walker, depending on the conditions. These tips help in fall prevention: – Handrails on the sides of stairways – Raised toilet seats with armrests – Sturdy seat for showers and hand-held shower nozzle Falls are largely preventable with the right awareness, support, and care. At the forefront of elderly fall prevention is MJ Naidu Hospital in Vijayawada, a trusted name in orthopedic excellence for over 40 years. Their team of specialists is dedicated to helping older adults stay mobile, confident, and safe. From advanced diagnostics to personalized rehabilitation and pain management, MJ Naidu Hospital offers a comprehensive approach to fall prevention and recovery, ensuring that every step forward is a safe one. Enquire now Table of Contents Causes of Falls in the Elderly Six Tips for Fall Prevention MJNaidu hospital latest Updates delivered straight to your inbox Follow Us You have been successfully Subscribed! Ops! Something went wrong, please try again.
Signs a Broken Bone Is Not Healing: What You Need to Know
Signs a Broken Bone Is Not Healing: What You Need to Know Facebook Twitter Youtube Instagram Worried about whether your broken bone is healing properly or not? If there is a delay in healing, then there could be a complication that may require medical attention. Knowing what symptoms to look for and how bone heals can help you determine if you need to take action to ensure a smoother recovery. Read the blog for the symptoms, stages of healing, and what to do if your bone is not healing to expectation. Understanding the 5 Stages of Bone Healing Let’s explain the 5 stages of bone healing so that you are aware of what is happening underneath that cast: Hematoma Formation (Days 1 – 7): Immediately following the fracture, blood pools at the fracture site, where a clot forms and begins the repair process. Inflammatory Stage (Week 1 – 2): Your body sends immune cells to the area to clean up debris and fight infection. This stage can be painful and swollen, but it indicates that your body is actively engaging with the process. Soft Callus Formation (Weeks 2 – 3): Blood starts forming a soft callus to heal around the fracture site. Hard Callus Formation (Weeks 4 – 8): That soft callus hardens into bone. Most individuals typically continue to wear a cast throughout this stage. Bone Remodeling (Months to years): Bone continues to slowly reshape, and get stronger as time passes. This process can occur over several months. Common Symptoms of Broken Bone Healing The time frame for healing can vary by age, bone type, and health status. Each stage of healing has some symptoms: Pain in broken bone regions decreases over time Very mild swelling or bruising at the injury site in the early stages Slight tingling or stiffness for some time after the broken bone has been immobilized for an extended time If you are noticing these signs and they are getting better, it means your body is healing properly. Signs a Broken Bone Is Not Healing Now, let’s get to the red flags. Here are the signs a broken bone is not healing properly: 1. Pain persists beyond the expected time frame There may be some mild discomfort associated with the healing bone and surrounding tissue, however, sharp or increasing pain present two to four weeks following the injury may suggest a problem exists. 2. Swelling does not reduce Swelling during your recovery may have some normal range, however, if swelling is sustained for more than two weeks (especially if warmth or redness is present) your bone may be at risk for malunion, delayed union, or nonunion where infection is present. 3. Abnormal movement at the fracture line If the fractured bone(s) feel unstable or have abnormal movement at the fracture line after completing weeks of treatment, it may indicate that the bone has not healed correctly. 4. Numbness or tingling You may be experiencing changes in sensation as part of your risk of nerve involvement. While it’s not necessarily related to the healing of the bone, it is something you should never ignore. 5. Loss of functional recovery Upon removal of your cast, you should begin to slowly experience functional return of strength and more range of motion. If you feel like you are stuck in recovery with no physical improvements, it may be the case that your bone is not healing properly. Do Broken Bones Heal Back to Normal? A common question is: Do fractured bones heal back to the normal path? In most cases, yes. fractured bones can heal back to their normal form with proper care. However, there are many variables involved: Age: Older adults fracture bones and heal slower. Type of bone: Weight-bearing bones (like the femur) can take longer because they are pressure-sensitive. Smoking or diabetes: Any smoker or diabetic can experience a healing delay. Poor immobilization: Moving the bone before its time can disturb the healing. You may be interested to know – Hairline Fracture What to Do If You Notice Signs a Broken Bone Is Not Healing? If you notice any symptoms that your broken bone is not healing, don’t ignore them. Pain that persists, swelling that lasts, and lack of bone healing can all be indications of a red flag. These symptoms could indicate that your bone is healing too slowly (or maybe not at all). Understanding the 5 stages of bone healing will help you track your healing. If you are not seeing improvement in broken bone healing symptoms, it’s time to take action. Here is what to do: 1. Consult Your Physician Do not guess! If something seems wrong, check with your doctor. They may send you for new X-rays or other tests to check the way your bone is healing. 2. Avoid Stressing the Bone Do not jump back to doing normal activities simply because the pain decreased. It is easy to stress your bone putting weight on it too soon, which can delay or even stop healing. 3. Enquire About Stimulation Some physicians use equipment to stimulate bone to heal such as low-level ultrasound or electric stimulation. 4. Consider Surgery In far fewer cases, a physician may consider surgery or a bone graph to fix the problem and help healing begin. Be aware, be vigilant, check your broken bone healing symptoms and also understand the 5 stages of bone healing to fully recover and heal safely.</span Trust the Experts in Bone Healing At MJ Naidu Super Specialty Hospital we recognize the importance of an appropriate diagnosis and prompt treatment for orthopedic care. With 38+ years of legacy, a team of celebrated orthopedic surgeons, and state-of-the-art services such as 24/7 trauma care, diagnostics, ICU, and operation theaters, we are dedicated to attaining patient-centric care through the combination of compassion and technology. Whether you are coping with fractures, joint problems, or complex bone pathologies, we are here for you. Enquire now Table of Contents Understanding the 5 Stages of Bone Healing Common Symptoms
PRP Injections for Knee Pain: A Revolutionary Treatment Option
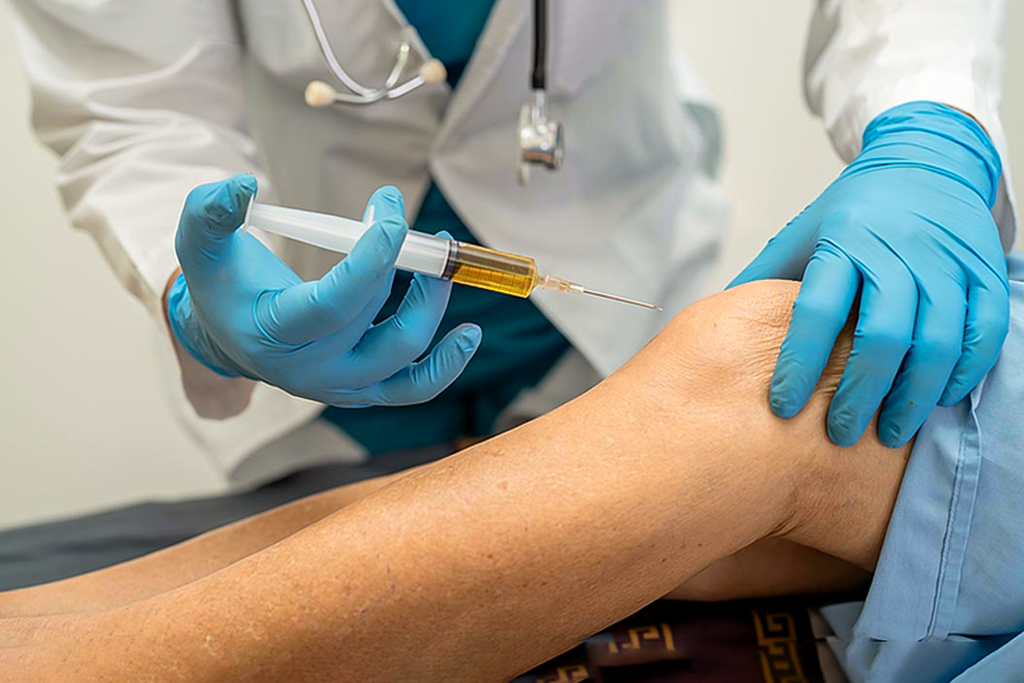
PRP Injections for Knee Pain: A Revolutionary Treatment Option Facebook Twitter Youtube Instagram Knee pain and tendon pain can be agonizing and not all times traditional techniques help. Knee pain is a frequent issue for athletes, often stemming from ligament strains, cartilage injuries, and tendonitis, as well as for individuals over 50 dealing with knee arthritis. What You Need to Know PRP injections offer effective support for wound healing in trauma and joint injuries. Results from PRP injections typically become noticeable within a few weeks for joint treatments. However, the effects are not permanent, and additional injections may be required as advised by a doctor. Since PRP injections utilize a patient’s tissues, they are considered safe and can be used as a standalone treatment or combined with other procedures for enhanced results. Platelet-rich plasma i.e. PRP injections for knee pain have been recognized for their ability to relieve joint pain, decrease inflammation, and enhance overall function. Both traumatic soft tissue injuries and degenerative conditions, such as meniscus deterioration, may benefit from this regenerative approach. PRP therapy is commonly used to treat knee osteoarthritis, tendon damage, patellar tendon injuries, and ligament issues like ACL tears. Research on PRP for knee osteoarthritis has consistently reported significant improvements in symptoms and recovery outcomes. Let’s dive in more to understand how PRP injections for knee pain work, what are the side effects, and when it is used. What is a PRP injection? Platelet-rich plasma is extracted from a patient’s blood sample and then carefully injected into the targeted area, like an injured knee or tendon. In some cases, ultrasound guidance is used to ensure precise placement. The goal is to boost the concentration of growth factors like special proteins and hormones at the site of injury, to accelerate natural healing. What is the procedure of administering a PRP injection? PRP therapy follows a three-step process: Blood Collection – A small amount of blood is drawn from your arm. Platelet Separation – The blood sample is placed in a centrifuge to isolate platelets, creating a concentrated plasma suspension. Injection – A doctor numbs your knee and injects the PRP directly into the joint space, possibly using ultrasound for precision. Why are PRP injections used? PRP injections are used for a variety of treatments, spanning musculoskeletal injuries, post-surgical recovery, and cosmetic procedures. Tendon, Ligament, Muscle & Joint Injuries – Chronic conditions like tennis elbow and jumper’s knee can take a long time to heal. PRP injections help accelerate recovery, reduce pain, and get patients back to their activities faster. Post-Surgical Healing – Originally used in jaw and plastic surgery, PRP injections are now aiding muscle, tendon, and ligament repair, helping patients recover from intensive procedures more efficiently. Osteoarthritis Relief – Early studies suggest PRP may reduce joint inflammation and stiffness, helping patients manage pain and improve mobility. Research is ongoing, but the results are promising. Benefits of taking PRP injections Accelerates healing of joint and sports injuries Reduces pain and inflammation Promotes natural tissue repair Enables faster return to physical activities Delivers noticeable results within a few months Minimally invasive and low risk Uses the patient’s own blood, making it a safe treatment option Suitable for chronic conditions like knee pain, tennis elbow, and jumper’s knee What are the risks and side effects associated with PRP injections for knee pain? PRP injections are generally low-risk and rarely cause major side effects. Since the procedure involves drawing blood, it’s important to stay hydrated and eat beforehand to avoid lightheadedness. Some soreness and bruising at the injection site are common after treatment. Because PRP uses your own plasma, the likelihood of an allergic reaction is much lower compared to other injectable medications like corticosteroids. While rare, potential risks include bleeding, tissue damage, infection, and nerve injuries. Consulting a healthcare professional can help ensure a safe and effective experience. Contact MJ Naidu to Schedule Your PRP Treatment PRP injections tap into your body’s natural healing power, offering safe, effective, and lasting relief from knee pain and stiffness. Whether you’re dealing with osteoarthritis, tendinitis, or other knee-related conditions, PRP injections for knee pain provide a promising, non-surgical solution to restore knee joint mobility and enhance your quality of life. At MJ Naidu, our team specializes in PRP injections to help you move with confidence again. Schedule your appointment today and take the first step toward pain-free living. https://www.youtube.com/shorts/ZIiIexJoeVs Frequently Asked Questions on PRP Injections 1. What is PRP? PRP (Platelet-Rich Plasma) is a concentrated solution of platelets from your own blood, rich in growth factors to promote healing. 2. How does PRP work? It works by injecting concentrated growth factors directly into an injured area, stimulating the body’s natural tissue repair and regeneration processes. 3. What is the PRP procedure? Blood is drawn, spun in a centrifuge to separate PRP, and then the concentrated PRP is precisely injected into the injured area. 4. What are the side effects? Common side effects are mild and temporary: pain, swelling, or bruising at the injection site. Serious complications like infection are rare. 5. How long does it take to work? Post PRP injection administration, the results are visible within 2-6 weeks, with continued improvement over several months, as tissue regeneration is a gradual process. 6. What are the applications for PRP for knee injuries? Common applications include knee osteoarthritis, meniscus tears, mild ligament sprains, and tendinopathies like “jumper’s knee.” Enquire now Relevant Resource : Hairline Fracture Table of Contents What is a PRP injection? What is the procedure of administering a PRP injection? Why are PRP injections used? Benefits of taking PRP injections What are the risks and side effects associated with PRP injections for knee pain? Contact MJ Naidu to Schedule Your PRP Treatment Frequently Asked Questions on PRP Injections MJNaidu hospital latest Updates delivered straight to your inbox Follow Us You have been successfully Subscribed! Ops! Something went wrong, please try again.
Understanding Arthroscopy: A Minimally Invasive Solution for Joint Pain and Injuries
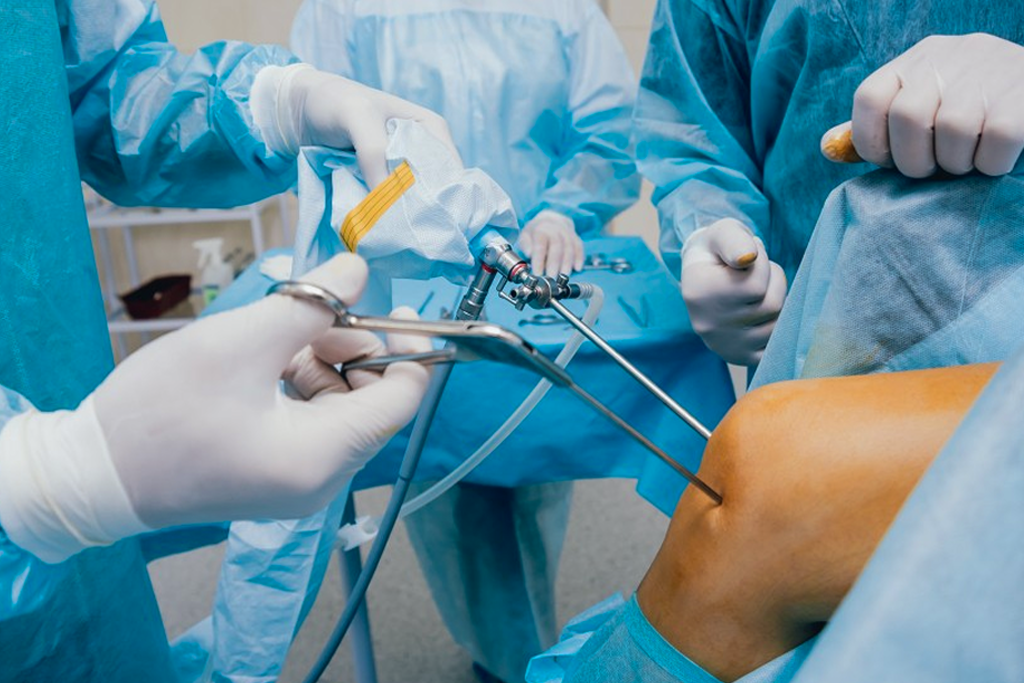
Understanding Arthroscopy: A Minimally Invasive Solution for Joint Pain and Injuries Facebook Twitter Youtube Instagram Are joint pains preventing you from getting around effectively or diminishing your daily tasks? Whether it’s a knee arthroscopy to repair a torn meniscus or shoulder arthroscopy for a rotator cuff injury, modern orthopedic surgery provides a unique and minimally invasive option. At MJ Naidu Super Speciality Hospital in Vijayawada, we specialize in utilizing arthroscopy to deliver effective and precise interventions for the various joint issues that keep you from enjoying life. All while experiencing quicker recovery times and less pain. Please read through the blog to discover how arthroscopy interventions can help you regain mobility, decrease pain, and enhance your life. What is Arthroscopy? Arthroscopy is a minimally invasive surgical technique for diagnosing and treating joint conditions. Instead of making large cuts, the surgeon visualises the joint using a small camera called an arthroscope and uses small instruments to repair any damage with great accuracy. Knee Shoulder Hip Ankle With our advanced technology and an experienced orthopedic surgeon, MJ Naidu is known as the place for arthroscopy in Vijayawada. How Arthroscopy Works? Anesthesia is used so that the procedure is comfortable and pain-free. The doctor makes a few small incisions around the affected joint. The doctor inserts an arthroscope to see inside the joint in high definition. The doctor may insert various surgical instruments to repair or remove damaged tissue. The incisions are closed, and the person begins to recover. What are the Advantages of Arthroscopy? Whether you’re looking at knee arthroscopy, shoulder arthroscopy, or arthroscopy in general, there are so many patient-focused benefits to surgical, minimally invasive arthroscopy that it is the top choice in today’s orthopedic practice: Minimally Invasive – The small incisions made by the orthopedic surgeon make injuries to localized and adjacent structures less likely. Faster Recovery – Patients undergoing knee or shoulder arthroscopy are more likely to heal and rehabilitate faster. Less Postoperative Pain – Although there is some discomfort involved, the small entry wounds are less painful than those associated with traditional open surgery. Lower Risk of Infection – The surgical wounds of arthroscopy are small, which means less surgeon-induced trauma, and thus less chance of infection. More Accurate Diagnosis – The high-definition imaging of the arthroscope will allow the orthopedic surgeon to accurately, in real-time, evaluate and diagnose the problems of the joint. Shorter Stay for Procedural Patients – Most joint arthroscopy cases are performed as outpatient procedures, meaning that a patient can go home the same day. Better Cosmetic Result – There may be some slight scars from shoulder arthroscopy and knee arthroscopy, but they are relatively small and not very noticeable. Cost-Effective – The less trauma experienced by patients’ tissues during surgery and the speed of recovery translate into reduced costs for the overall treatment of the injury. Improved Joint Function – The arthroscopic procedure will allow the orthopedic surgeon to address the specific problem accurately, which means that joint mobility can be restored almost immediately following surgery to obtain a sustainable return to the rehabilitative process. Wide Range of Applications – The range of joint conditions that can be addressed using arthroscopic surgery includes isolated meniscus repairs, as well as rotator cuff injuries, among other common injuries. Knee Arthroscopy: Targeted Treatment for Everyday Problems Knee arthroscopy is one of the most commonly performed orthopedic procedures—and for good reason. The knee is one of the most used and at-risk joints of the body. At MJ Naidu, we use knee arthroscopy to treat: Meniscus tears ACL injuries Loose bone fragments Cartilage wear and damage Knee joint infections Why Have Knee Arthroscopy? Smaller incisions, less pain Minimal scarring Quicker recovery compared to open surgery Accurate diagnosis and treatment in a single operation If you’ve been putting off knee surgery due to fears of prolonged recovery or pain, knee arthroscopy may be the best option available to you. With qualified orthopedic surgeons and contemporary surgical theatres, MJ Naidu guarantees the best results with the least amount of discomfort. Shoulder Arthroscopy: A Minimally Invasive Solution for Shoulder Pain Shoulder arthroscopy has become another revolutionary procedure for the treatment of acute injuries and chronic conditions related to the shoulder. Whether you play sports, work in an office, or are elderly, shoulder issues can severely impact your daily life. At MJ Naidu, shoulder arthroscopy is commonly conducted to treat: Rotator cuff tears Frozen shoulder Shoulder impingement Labral tears Recurrent dislocations Our orthopedic specialists use state-of-the-art technology, so you can be assured that your shoulder is treated with skill and precision, resulting in faster rehabilitation and long-term pain relief. Post-Arthroscopy Recovery and Rehabilitation As a minimally invasive procedure, recovery after arthroscopy is usually much smoother and faster than open surgery. Arthroscopy procedures include knee arthroscopy, shoulder arthroscopy and others; regardless of the joint type involved, the most important factor in recovery following arthroscopy is adhering to the full physiotherapy rehabilitation plan, so you can fully heal and protect the long-term function of your joint. The general advice when recovering from any procedure is to rest the joint and use ice for swelling, combined with a specific physiotherapy program. For knee arthroscopy, the focus of rehabilitation will involve returning the missing strength, balance and flexibility to your leg. For recovery following shoulder arthroscopy, rehabilitation will focus on restoring mobility, stability, and range of motion to your shoulder. At MJ Naidu Super Speciality Hospital, we have an incredible, knowledgeable team that will assist you through every single step of your recovery and rehabilitation journey to facilitate your return to everything you love to do as quickly and safely as possible. Schedule An Arthroscopy Consultation With Us Today If you’ve been searching online for arthroscopy, knee arthroscopy, or shoulder arthroscopy, the team at MJ Naidu Super Speciality Hospital in Vijayawada is ready to help. The aspects of clinical excellence and compassion (care) ensure that patients receive the best treatment for their unique condition. Are you ready to take the first step towards a life
Osteoporosis in Women: Why It’s More Common and How to Prevent It

Osteoporosis in Women: Why It’s More Common and How to Prevent It Facebook Twitter Youtube Instagram According to the World Health Organization (WHO), osteoporosis is diagnosed when bone density falls below 2.5 SD (standard deviation) compared to a healthy population of the same age and gender. Osteoporosis impacts the physical, emotional, and mental well-being of postmenopausal women and also leads to reduced bone density and quality, making bones more porous and fragile. This results in women with osteoporosis prone to a higher risk of fractures, even from minor slips, falls, or, in some cases. Osteoporosis affects one in three women and one in five men over the age of 50. WHO Criteria for Osteoporosis Using BMD (Bone Mineral Density) Classification by T-Score Value: Normal: Greater than -1.0 Osteopenia: -1.0 to -2.5 Osteoporosis: Less than -2.5 Severe or Established Osteoporosis: Less than -2.5 with a history of fragility fractures What is Osteoporosis? Osteoporosis is a condition that weakens bones, makes them brittle, and prone to fractures. Often, it develops silently, with no noticeable symptoms until a bone breaks. It is characterized by low bone density and structural deterioration, leaving bones vulnerable to damage from minor falls or even routine movements. What causes Osteoporosis? Osteoporosis is commonly seen in older women, but it is not exclusively tied to aging. Many underlying conditions contribute to what causes osteoporosis, even in younger women. Medical Conditions That Increase Risk – Certain diseases have strong links to osteoporosis symptoms, including: Hyperthyroidism Hyperparathyroidism Celiac disease Chronic kidney disease Autoimmune disorders like rheumatoid arthritis, SLE (systemic lupus erythematosus), and ankylosing spondylosis Lifestyle Factors & Modifiable Risks – Smoking and excessive alcohol intake are significant contributors to what causes osteoporosis and can worsen osteoporosis symptoms. Reducing these habits plays an essential role in osteoporosis prevention. Vitamin D & Bone Health – Vitamin D is crucial for calcium absorption and overall bone strength. Lack of sunlight exposure, especially in regions with limited tropical weather can contribute to osteoporosis symptoms and increase fracture risk. Medication-Induced Osteoporosis – The careful use of certain medications is necessary, as they are known secondary risk factors for osteoporosis treatment and osteoporosis prevention. These include: – Corticosteroids – Thyroxine – Antacids – Chemotherapy drugs, especially aromatase inhibitors By addressing these risk factors early and making lifestyle adjustments, osteoporosis prevention becomes more effective, reducing the likelihood of developing severe osteoporosis symptoms later in life. https://youtube.com/shorts/bx-9NLqrbVU?feature=shared What are the osteoporosis symptoms? Osteoporosis symptoms often go unnoticed in the early stages, as bone loss occurs gradually. However, once bones become weak, noticeable signs may develop, like the following osteoporosis symptoms: – Persistent back pain, often caused by fractures or collapsed vertebrae. – Loss of height over time due to weakened spinal bones. – A stooped posture, resulting from poor bone strength. – Fragile bones that break more easily than expected, even from minor falls or pressure. Recognizing osteoporosis symptoms early can help in managing the condition effectively and reducing fracture risk. What can be done for osteoporosis prevention? While osteoporosis when develops often goes unnoticed, taking proactive steps toward osteoporosis prevention can help maintain strong, healthy bones throughout life. Why Osteoporosis Prevention Matters Bone loss is a natural process that accelerates with age; factors such as poor diet, lack of physical activity, smoking, and excessive alcohol consumption increase the risk of developing osteoporosis. The good news? Osteoporosis prevention is possible with simple daily habits. Key Tips to Prevent Osteoporosis #Tip1 Osteoporosis Prevention: Prioritize Calcium & Vitamin D Intake Calcium is essential for bone health, while vitamin D helps with calcium absorption. Incorporate calcium-rich foods like dairy, leafy greens, and fortified products into your diet. For vitamin D, ensure adequate sun exposure or take supplements if necessary. #Tip2 Osteoporosis Prevention: Stay Active with Weight-Bearing Exercises Regular exercise strengthens bones and improves overall stability. Engage in weight-bearing activities such as walking, jogging, dancing, or resistance training. These exercises help slow bone loss and enhance density, making them an important part of osteoporosis prevention. #Tip3 Osteoporosis Prevention: Quit Smoking & Limit Alcohol Consumption Smoking weakens bones and decreases bone mass over time, increasing the risk of fractures. Excessive alcohol consumption interferes with calcium absorption and hormone regulation, making osteoporosis more likely. #Tip4 Osteoporosis Prevention: Maintain a Balanced Diet A well-rounded diet with essential nutrients like magnesium, potassium, and protein contributes to stronger bones. Processed foods and excessive caffeine intake can reduce calcium absorption, so focus on whole, nutrient-dense meals to support osteoporosis prevention. #Tip5 Osteoporosis Prevention: Prevent Falls & Reduce Fracture Risk Falls are a leading cause of fractures in people with osteoporosis. Simple safety measures, such as keeping living spaces well-lit, removing trip hazards, and practicing balance exercises like Tai Chi, can significantly reduce the risk of injury. #Tip6 Osteoporosis Prevention: Get Regular Bone Density Check-Ups Routine bone density screenings help detect early signs of osteoporosis, allowing for timely intervention. If needed, medications may be prescribed to slow bone loss and strengthen the skeletal system. What is involved in osteoporosis treatment? A checklist Bisphosphonates such as Alendronate, Risedronate, and Zoledronic Acid are commonly prescribed medications for osteoporosis treatment. Denosumab (Prolia) may be recommended for individuals who cannot tolerate bisphosphonates. Hormone-related therapies like Estrogen and Raloxifene can help manage bone loss. Ensuring adequate calcium and vitamin D intake is crucial for maintaining bone strength. Weight-bearing and muscle-strengthening exercises support bone health and reduce osteoporosis symptoms. Quitting smoking and limiting alcohol consumption can lower the risk of fractures. Fall prevention strategies at home, such as improving lighting and removing hazards, help prevent fractures. Using proper lifting techniques can minimize strain on bones and reduce fracture risks. Regular bone density tests allow early detection and monitoring of osteoporosis progression. Consulting a healthcare provider to discuss long-term medication plans ensures effective osteoporosis treatment. Start your healthy knee journey today with MJ Naidu Hospital With over 38 years of excellence, MJ Naidu has established itself as a trusted name in healthcare, delivering expert
7 Gentle Knee Replacement Exercises to Restore Mobility After Surgery

7 Gentle Knee Replacement Exercises to Restore Mobility After Surgery Facebook Twitter Youtube Instagram Recovery after knee surgery is crucial and must be paired with vigorous knee replacement exercises apart from focusing on nutrient rich diet. After your knee surgery, you’ll likely feel pretty good for the first day due to the effects of the medicine. If your surgery was to address painful arthritis, the recovery might be less uncomfortable than expected, and the discomfort will gradually reduce over time. Physical therapy exercises for the knee after surgery follows a step-by-step approach. First, during the initial six weeks, the focus is on improving your range of motion. Next, between weeks six and sixteen, you do knee replacement exercises focused on rebuilding strength in your knee. Finally, therapy is tailored to your personal goals, whether it’s walking comfortably, playing with family, or getting back to sports. This structured process helps you regain mobility and achieve a successful recovery. Why Post-Knee Replacement Exercises Matter? Engaging in the right exercises after knee replacement is critical for recovery. These exercises improve mobility, reduce stiffness, and strengthen muscles around the knee, enabling patients to regain independence and perform daily activities with ease. With regular knee replacement exercises you can experience enhanced circulation, promote healing, and minimize the risks of complications. A consistent knee replacement exercises regimen ensures flexibility, joint strength, and long-term success while boosting confidence in adapting to new movements. 7 Gentle Knee Replacement Exercises for Post Surgery Recovery Before starting off, you must have a structured plan of physical therapy exercises for knee recovery. Early-stage knee replacement exercises like ankle pumps, quadriceps sets, and heel slides help reduce stiffness, improve blood flow, and rebuild muscle strength. These foundational knee replacement exercises prepare your joint for advanced movement and promote optimal healing. With consistent and proper knee replacement exercises, patients achieve improved mobility, strength, and quality of life. With regular practice, you will experience a smooth recovery and will also prevent future complications. #1 Knee Replacement Exercises Active Knee Slides Place a plastic bag under your operated foot to reduce friction while performing the movements. Bend your knees as far back as is comfortable, holding the position for 20-30 seconds. Initially, this may feel painful or tight, but this is normal, and both pain and flexibility will improve with time. Exercise guidance: Perform 5 repetitions, 4-5 times daily. #2 Knee Replacement Exercises Static Quads Lie on your back or sit with your legs stretched out straight. Point your toes towards your shins and press your knees firmly into the bed or surface. Hold the contractions for 10 seconds and then relax. These knee replacement exercises strengthen your thigh muscles and improve knee stability. Exercise guidance: Perform 6 repetitions, 4-5 times daily. #3 Knee Replacement Exercises Inner Range Quads In a long sitting position with towels under your knees, stretch your legs straight. Pull your toes toward your shins and press your knees down into the towels, lifting your feet slightly off the surface. Hold the position for 5-10 seconds and relax. These knee replacement exercises help improve muscle strength and joint function. Exercise guidance: Perform 6 repetitions, 4-5 times daily. #4 Knee Replacement Exercises Straight Leg Raises Lie on your back with your operated legs out straight. Pull your toes toward your shins and keep your knees straight as you lift your legs approximately 20cm off the surface. Hold for 5-10 seconds and then gently relax. These physical therapy exercises for knees are vital for strength building. Exercise guidance: Perform 5 repetitions, 4-5 times daily. #5 Knee Replacement Exercises Sitting Knee Hangs on Stools Sit on a chair with your legs supported on another chair. Actively straighten your legs in this position by pushing your knees downward, holding them for 20-30 seconds. This is one of the many helpful knee replacement exercises for enhancing flexibility. #6 Knee Replacement Exercises Hamstring Stretches on Stairs Place your operated legs on the bottom stair or a footstool. Pull your toes toward your shins while pushing your heels down and trying to straighten your knees. Lean your upper body forward slightly to feel a stretch behind your knees and thighs. These stretches complement other knee replacement exercises for recovery.Exercise guidance: Perform 4-5 repetitions daily. #7 Knee Replacement Exercises Wall Squat Holds Stand with your feet shoulder-width apart, slightly angled outward. For support, hold onto a chair if needed. Slowly lower yourself down the wall, keeping your back against it, and pause in the squat position for 5-10 seconds before returning to the starting position. These advanced knee replacement exercises build muscle strength and joint stability. Exercise guidance: Perform 6 repetitions, 4-5 times daily. Practicing these knee replacement exercises consistently will enhance mobility, strength, and flexibility. Following structured physical therapy exercises for knees ensures a smoother recovery and long-term joint stability. Image source: NHS UK FAQs on Knee Replacement Exercises 1. What are the most important knee replacement exercises? The most important knee replacement exercises include ankle pumps and knee extensions, which help improve blood circulation and restore range of motion early in recovery. 2. How can I regain my mobility after knee surgery? Mobility can be regained through consistent knee replacement exercises like heel slides, straight-leg raises, and walking with support, which strengthens muscles and improves flexibility. 3. How to loosen tight muscles after knee replacement? To loosen tight muscles, focus on gentle knee replacement exercises such as static stretches, quadriceps sets, and using a stationary bike to gradually improve flexibility. 4. How many days of physiotherapy after knee replacement? Physiotherapy after knee replacement typically lasts 12 weeks, with knee replacement exercises tailored to each recovery phase, and may extend further based on individual progress. 5. How long does it take to walk normally after total knee replacement? Walking normally after a total knee replacement can take around 6 to 12 weeks, depending on individual recovery and consistent practice of knee replacement exercises. 6. What is the hardest part of knee replacement recovery? The hardest part of

